Surgical Approach
Minimally Invasive Foot & Ankle Surgery
Smaller incisions. Less soft tissue disruption. Faster recovery. Minimally invasive techniques allow many foot and ankle conditions to be corrected with significantly less trauma than traditional open surgery.
Dr. Bregman performs minimally invasive bunion correction (Bunionplasty MIS), minimally invasive hammertoe correction, and other minimally invasive procedures. Not every patient is a candidate — a thorough evaluation determines the most appropriate surgical approach for each individual case.
The Advantages
Why Minimally Invasive When Appropriate
Smaller Incisions
Incisions of 2–5mm versus the 5–8cm incisions used in traditional open surgery. Less visible scarring and reduced risk of wound complications.
- 2–5mm incisions
- Minimal visible scarring
- Reduced wound complication risk
Less Soft Tissue Disruption
Specialized instruments work through small portals without the extensive soft tissue dissection required in open surgery. This preserves blood supply and reduces post-operative swelling.
- Preserved blood supply
- Reduced post-operative swelling
- Less tissue trauma
Faster Recovery
Most patients are walking in a surgical shoe immediately after minimally invasive bunion surgery. Return to normal footwear is typically faster than with traditional open procedures.
- Walk same day (surgical shoe)
- Faster return to footwear
- Earlier return to activity
Actual Patient Results
Before & After: Minimally Invasive Bunion Correction
The following X-rays and clinical photos are from Dr. Bregman's own patients. Note the dramatic bone realignment on X-ray — and on the clinical photos, the incisions are so small they are almost invisible.
Case 1 — Clinical Photos: Post-Operative Results
Both photographs below are post-operative images from the same patient, taken at different angles to demonstrate the near-complete absence of visible scarring following minimally invasive bunion surgery.
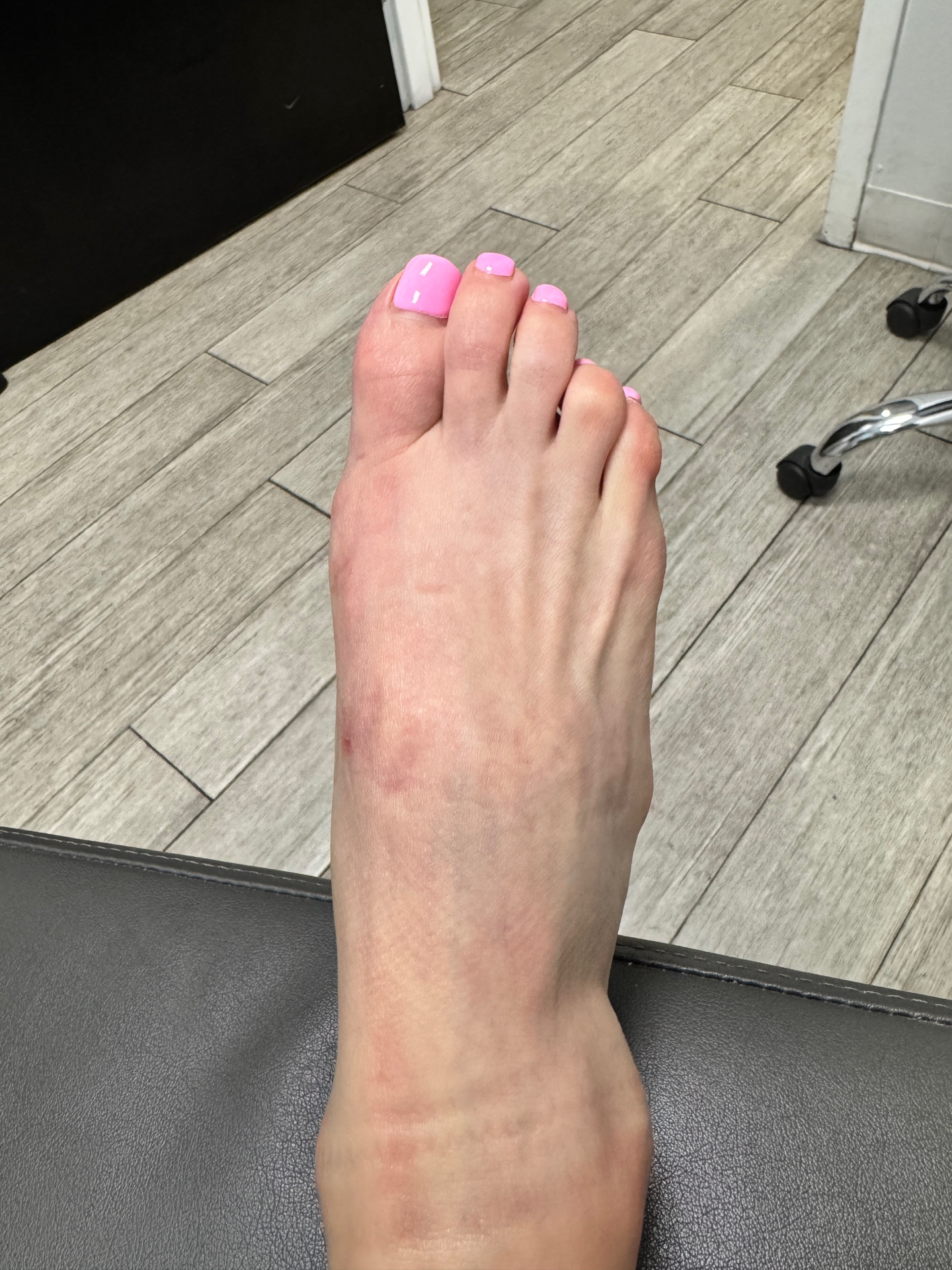
Post-operative result — incisions virtually invisible
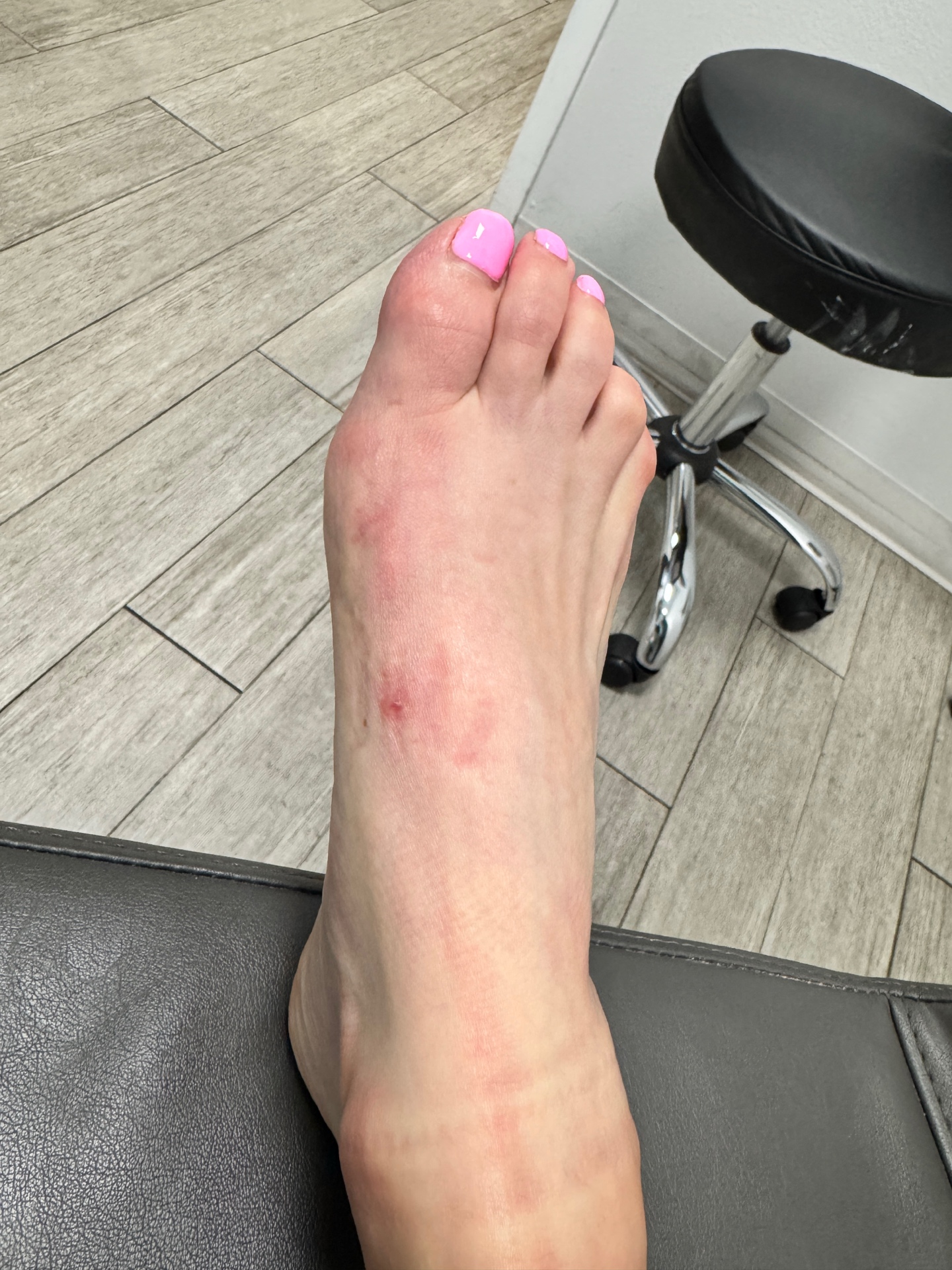
Corrected alignment — scarring almost entirely absent
Case 1 — X-Rays: Bone Realignment
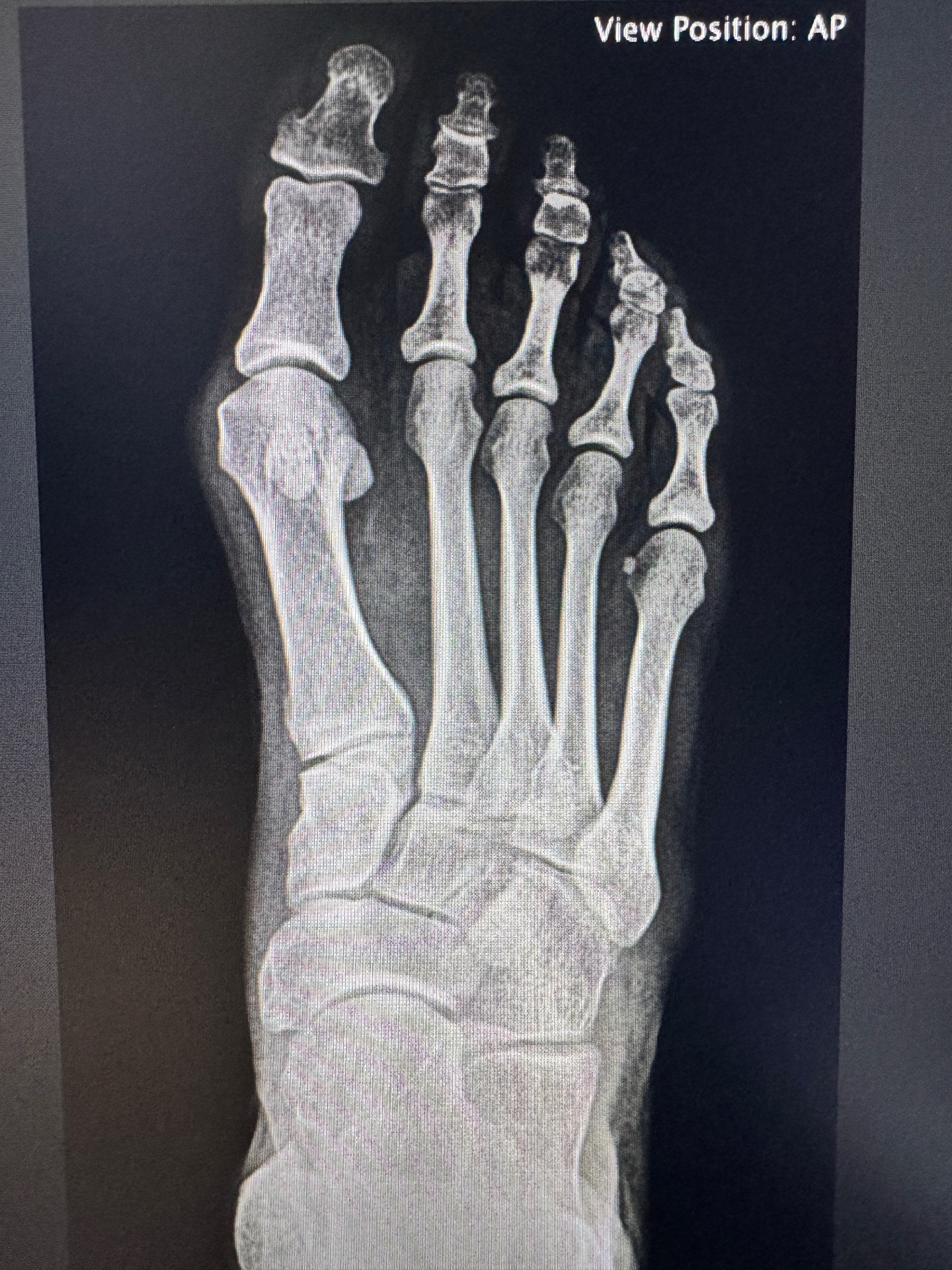
AP weight-bearing X-ray — hallux valgus deformity with metatarsal deviation
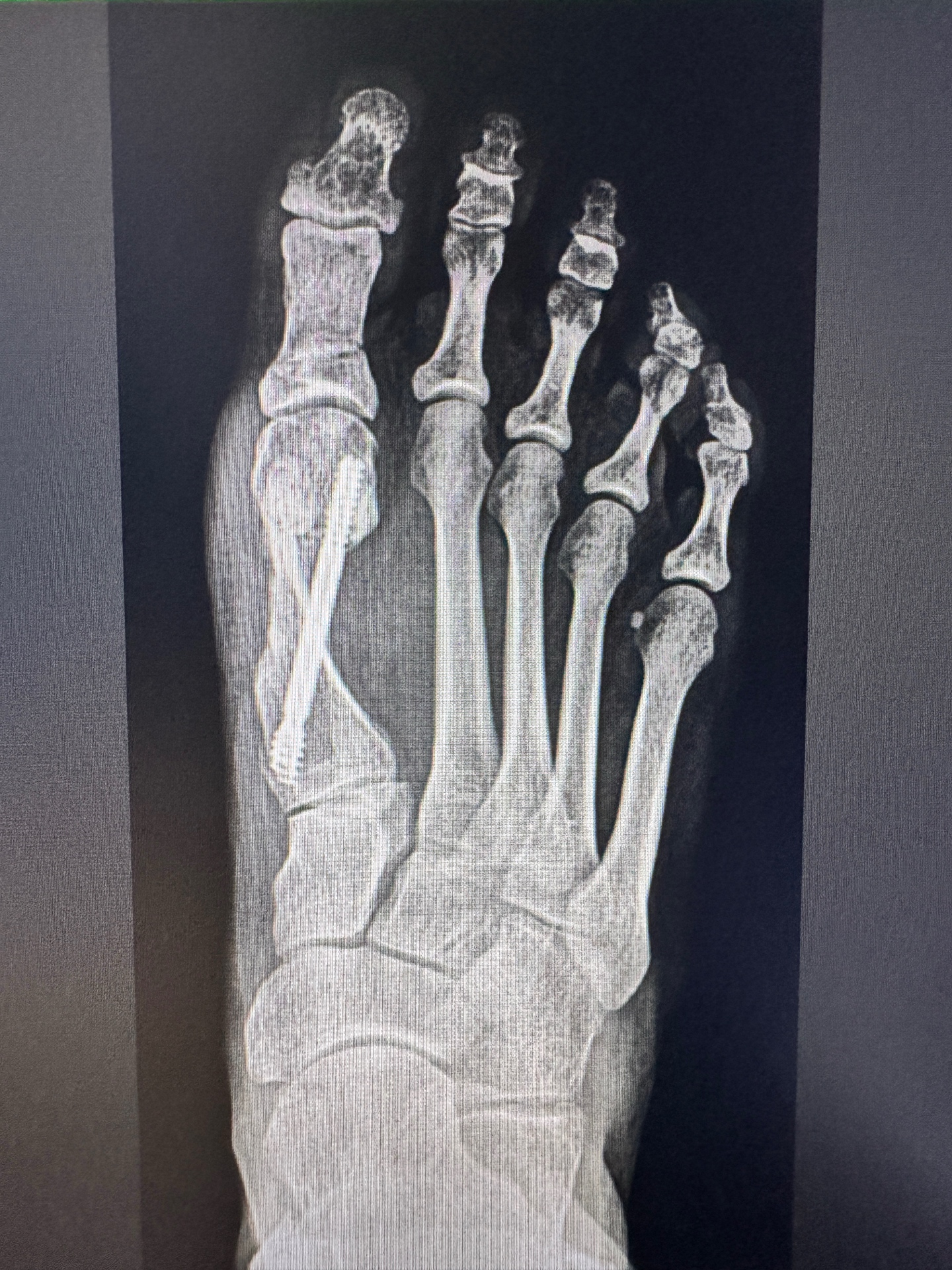
Corrected alignment — internal fixation screw visible, first metatarsal realigned
Case 2 — X-Rays: Bunion Correction
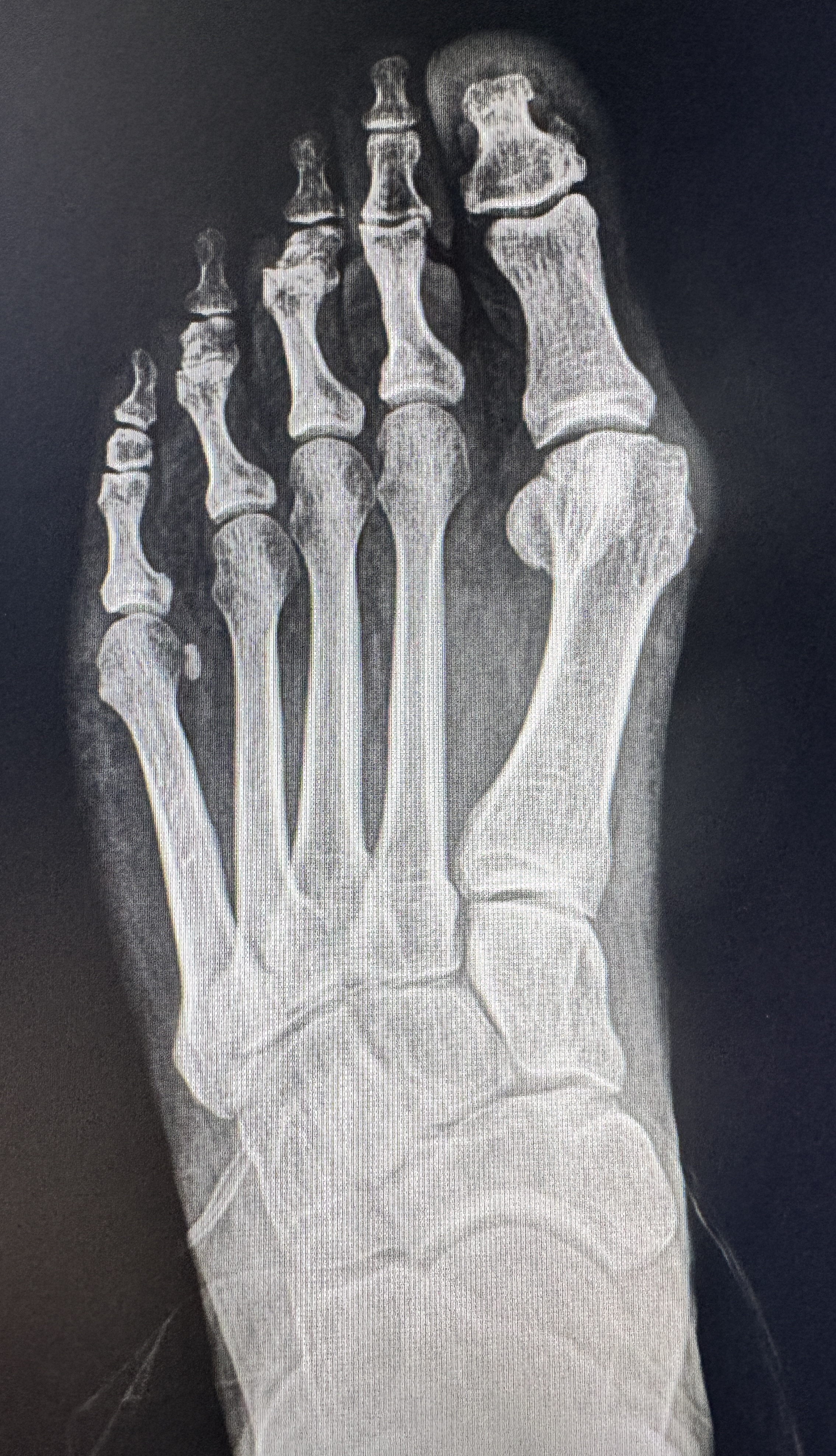
Significant hallux valgus deformity with lateral toe crowding
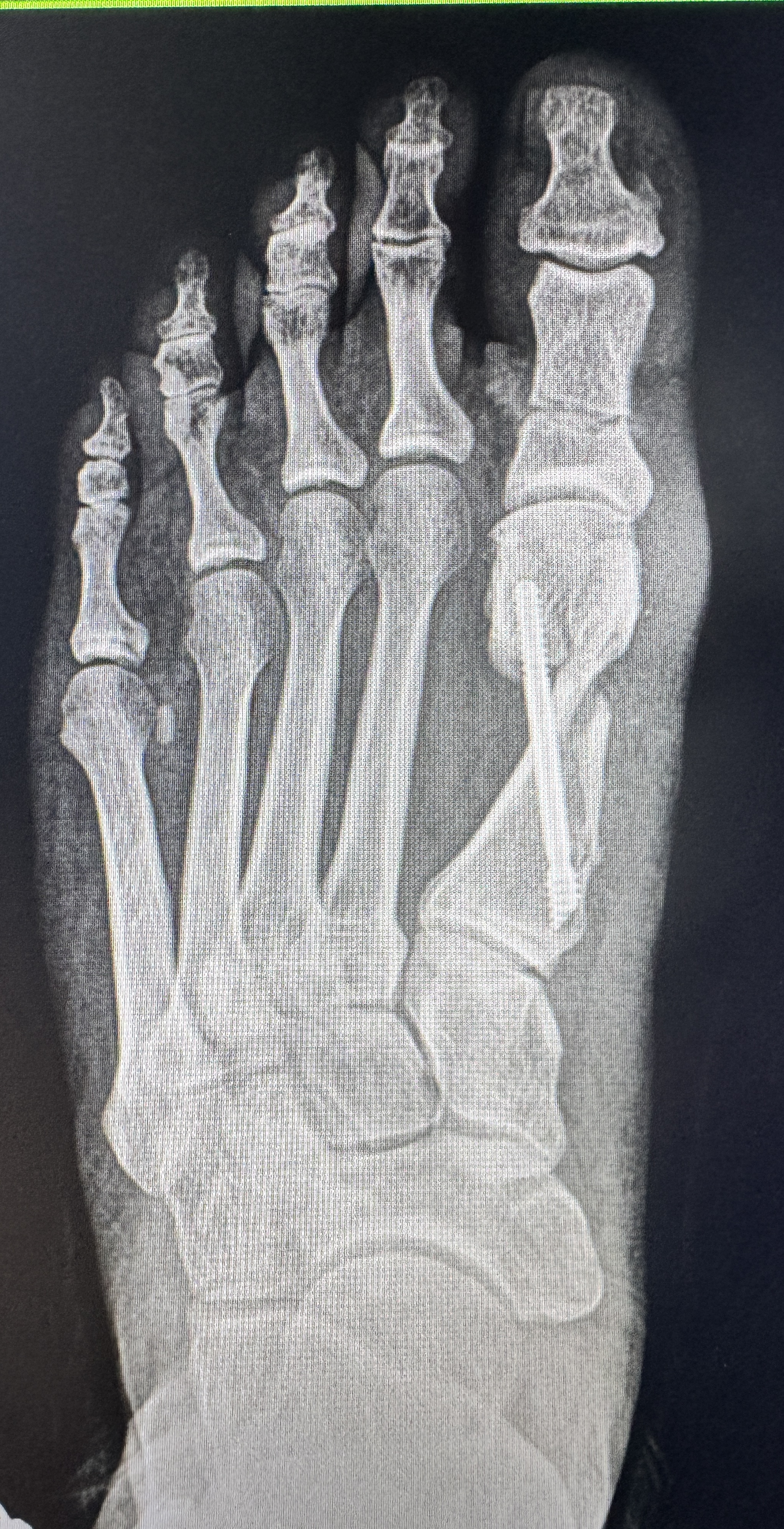
Excellent realignment — fixation hardware placed through minimal incisions
Case 3 — X-Rays: Before & After Bunion Correction
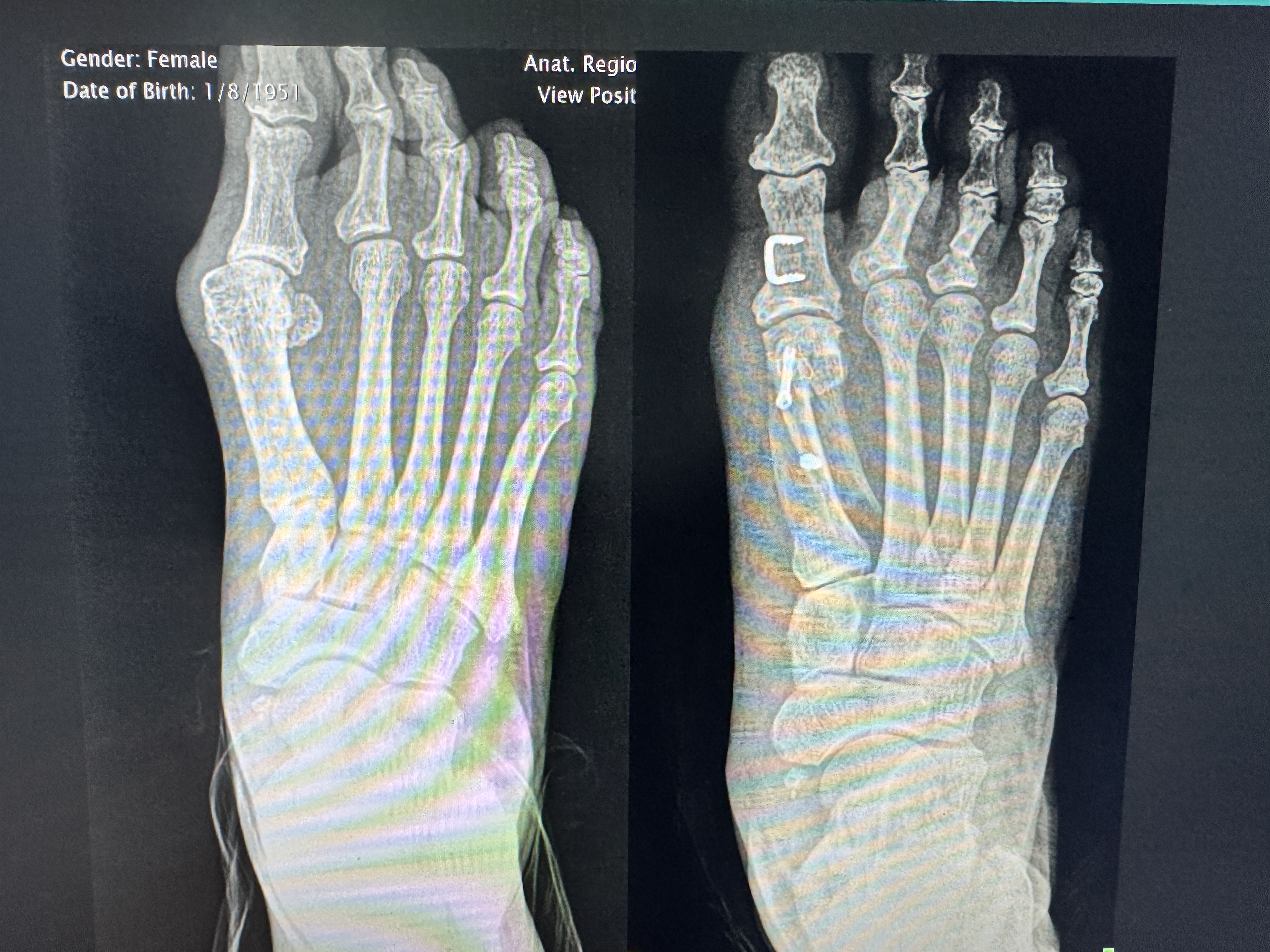
Female patient. Dramatic realignment of the first metatarsal achieved through minimally invasive technique.
Separate Patient — Video Follow-Up
6 Weeks After Minimally Invasive Bunion Surgery
At just six weeks post-operatively, this patient demonstrates near-complete scar disappearance — the incisions are barely visible. Full range of motion is present and the patient reports zero pain. This is a different patient from the X-ray cases above.
6-week post-op follow-up — scar nearly invisible, full range of motion, no pain. Minimally invasive bunion surgery by Dr. Peter J. Bregman, DPM.
Notice on the clinical photos: the incisions are so small they are almost invisible — yet the X-rays show complete correction of the bone deformity. This is the power of minimally invasive technique in the right hands.
Patient photos: Images are from Dr. Bregman's actual patients and are shared with consent for educational purposes. Individual results vary. A thorough evaluation is required to determine candidacy for minimally invasive surgery.
Bone Healing Process
From Surgery to Full Healing: A Visual Walkthrough
This video walks through the complete bone healing journey following minimally invasive bunion surgery — from the immediate post-operative state through progressive bone consolidation to full healing. Understanding what your bones are doing at each stage helps set realistic expectations and reinforces the importance of following post-operative protocols.
Video walkthrough: bone healing progression after minimally invasive bunion surgery — from post-operative day 1 through complete bone consolidation. Presented by Dr. Peter J. Bregman, DPM.
Procedures
Minimally Invasive Procedures Offered
Minimally Invasive Bunion Correction (Bunionplasty MIS)
Correction of hallux valgus (bunion) deformity using small incisions and specialized burrs. The bone is remodeled and repositioned through 2–3 small portals. Performed as an outpatient procedure. Most patients walk immediately in a surgical shoe.
Candidacy note: Mild to moderate bunion deformities. Severe deformities may require open correction.
Minimally Invasive Hammertoe Correction
Correction of hammertoe, claw toe, and mallet toe deformities through small incisions. Tendon releases, joint releases, and bone procedures can be performed with minimal soft tissue disruption.
Candidacy note: Flexible and semi-rigid hammertoe deformities. Rigid deformities may require open correction.
Minimally Invasive Plantar Fascia Release
Endoscopic or percutaneous release of the plantar fascia for chronic plantar fasciitis that has not responded to conservative treatment. Performed through one or two small incisions.
Candidacy note: Chronic plantar fasciitis (>6 months) that has failed conservative treatment. Nerve entrapment must be ruled out first.
Minimally Invasive Nerve Decompression
Decompression of entrapped nerves (Morton's neuroma, tarsal tunnel) through small incisions using specialized instruments. Preserves nerve function while relieving compression.
Candidacy note: Confirmed nerve entrapment that has not responded to conservative treatment.
Common Questions
Frequently Asked Questions
What is minimally invasive foot surgery?
Minimally invasive foot surgery uses small incisions (typically 2–5mm) and specialized instruments to correct deformities and treat conditions that traditionally required larger open incisions. The goal is to achieve the same or better correction with less soft tissue disruption, less pain, and faster recovery.
Am I a candidate for minimally invasive bunion surgery?
Candidacy for minimally invasive bunion surgery depends on the severity and type of your bunion deformity, bone quality, and other individual factors. A thorough evaluation including weight-bearing X-rays is required to determine whether minimally invasive correction is appropriate for your specific case.
What is the recovery like after minimally invasive bunion surgery?
Most patients are walking in a surgical shoe immediately after minimally invasive bunion surgery. Return to normal footwear typically occurs at 6–8 weeks. Full recovery and return to all activities varies by individual but is generally faster than with traditional open bunion surgery.
Is minimally invasive surgery always better than open surgery?
Not necessarily. Minimally invasive techniques are appropriate for certain cases and certain deformities. For complex or severe deformities, traditional open surgery may provide more reliable correction. Dr. Bregman evaluates each case individually and recommends the approach most likely to achieve the best outcome.
What is Bunionplasty MIS?
Bunionplasty MIS is a specific minimally invasive bunion correction technique that uses small incisions and specialized burrs to remodel the bone and correct the deformity. It is performed as an outpatient procedure under local or regional anesthesia.
Find Out If You Are a Candidate
A thorough evaluation including weight-bearing X-rays is required to determine whether minimally invasive surgery is appropriate for your specific condition and deformity.