Adult Flat Feet Treatment
Adult acquired flatfoot deformity is a progressive condition that can lead to significant pain and disability if left untreated. Dr. Bregman provides a comprehensive, individualized approach — from advanced orthotics to minimally invasive surgical correction.
Understanding Adult Acquired Flatfoot
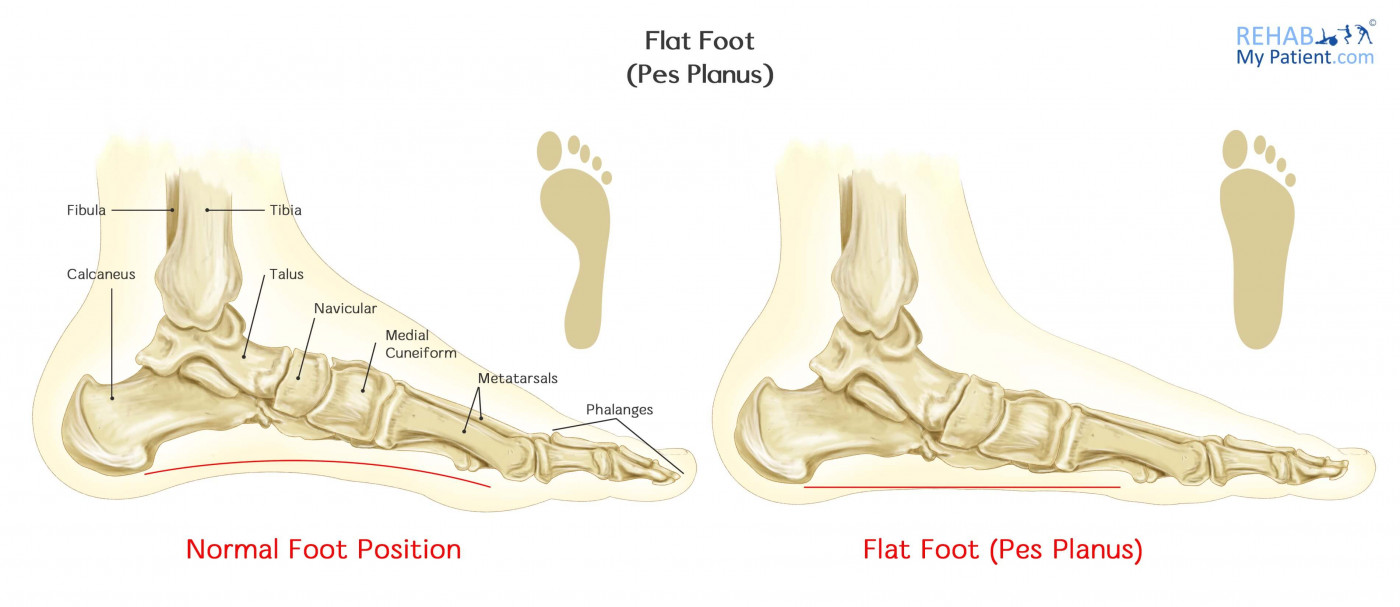
Unlike childhood flat feet, adult acquired flatfoot deformity (AAFD) develops over time — most commonly due to dysfunction or rupture of the posterior tibial tendon, the primary tendon responsible for supporting the arch. As the tendon weakens, the arch progressively collapses, causing the foot to roll inward (pronate) and the heel to shift outward.
AAFD is more common in women and adults over 40, and is strongly associated with obesity, hypertension, diabetes, and prior ankle injuries. Without treatment, the deformity worsens and can affect the ankle, knee, and hip.
Many patients are told to "just wear supportive shoes" — but this approach does not address the underlying tendon pathology or prevent progression.
Signs & Symptoms
Pain along the inner ankle and arch
Especially with walking or standing for extended periods
Visible collapse of the arch
The foot appears flat when standing
Heel shifting outward
The heel tilts away from the midline (valgus alignment)
Difficulty rising on tiptoes
A key clinical sign of posterior tibial tendon dysfunction
Swelling along the inner ankle
Along the course of the posterior tibial tendon
Progressive worsening
Symptoms worsen over months to years without treatment
The 4 Stages of Adult Flatfoot Deformity
Tendon Inflammation
Posterior tibial tendon is inflamed but intact. Arch is still present. Treated conservatively.
Flexible Flatfoot
Tendon is elongated or partially torn. Arch collapses under weight but can be corrected manually. Most common stage.
Rigid Flatfoot
Arch collapse is fixed — the foot cannot be corrected manually. Arthritis may be present.
Ankle Involvement
Deformity has progressed to involve the ankle joint. Surgical reconstruction typically required.
Dr. Bregman's Treatment Approach
Non-Surgical Options
Surgical Options (Stages II–IV)
Frequently Asked Questions
Can adult flat feet be corrected without surgery?
In Stage I and Stage II (flexible) flatfoot, conservative treatment — including custom orthotics, regenerative medicine, and physical therapy — can significantly reduce pain and slow progression. Surgery is typically reserved for cases that fail conservative treatment or have progressed to Stage III or IV.
How do I know if my flat feet are causing my pain?
Dr. Bregman performs a comprehensive biomechanical evaluation including weight-bearing X-rays, gait analysis, and clinical testing of the posterior tibial tendon. This allows precise staging and treatment planning.
Will my flat feet get worse over time?
Without treatment, adult acquired flatfoot deformity is progressive. Early intervention — even with conservative measures — can significantly slow or halt progression.
How long is recovery from flat feet surgery?
Recovery depends on the procedure. Tendon transfer with calcaneal osteotomy typically requires 6–8 weeks non-weight-bearing, followed by progressive rehabilitation over 3–6 months. Dr. Bregman uses regenerative medicine and peptide therapy post-operatively to accelerate healing.
Frequently Asked Questions
Common questions about flat feet treatment in Las Vegas
Don't Let Flat Feet Hold You Back
Schedule a comprehensive evaluation with Dr. Bregman to determine the stage of your flatfoot deformity and the best treatment path for your lifestyle.
Request a Consultation